
Choosing to implement a gluten-free and dairy-free diet for a child with autism can be beneficial in many ways.
Reports from parents include improvements in cognition, receptive and expressive language, development, skin conditions, as well as reduction in behaviors, improved sleep, decreased ear infections and digestive symptoms, and more.
If you have heard there is “no science” behind a gluten-free and dairy-free diet for autism, it’s just not true.
Thousands of anecdotal reports from parents plus existing scientific data shows that following this diet can help children with autism.
Understanding the potential impact of an autism diet plan is especially important in considering this option for your child.
What Is Gluten?
 Gluten is the term for the proteins found in wheat, barley, rye, and triticale, and products made from them. Gluten helps different foods maintain their shape by acting as a “glue” that holds things together. You can find gluten in various foods, such as soups, pasta, baked goods, cereals, processed meats, dressings, and sauces.
Gluten is the term for the proteins found in wheat, barley, rye, and triticale, and products made from them. Gluten helps different foods maintain their shape by acting as a “glue” that holds things together. You can find gluten in various foods, such as soups, pasta, baked goods, cereals, processed meats, dressings, and sauces.
Exposure to gluten can also come from what is called “cross-contamination.” This is when a gluten-free food is prepared, heated, fried, or placed with foods that contain gluten. Common sources of cross-contamination include French fries that are fried in the same fryer with gluten containing foods like breaded chicken or fish patties, as well as toasters, cutting boards, even knives.
The more sensitive the individual is, the more they will react to these cross-contamination situations. Have a separate toaster, cutting board, and knives for gluten-free cooking/prep and thoroughly wash all surfaces.
Thoroughly researching the different foods that contain gluten and possible risks of cross-contamination is important when following a gluten-free diet for autism.
Dairy / Casein
Dairy is a term that refers to all animal milk and milk products, and is made up of different components (for example, lactose is the milk sugar).
Casein is a type of protein in milk.
Just as with gluten, you can have cross-contamination with dairy, so use the same cross-contamination precautions regarding cutting boards, counters, etc.
If something is made from dairy, it could contain casein (unless it says “casein-free”). Often the terms “dairy-free” and “casein-free” are used interchangeably. When reading labels, we often assume dairy-free means casein-free (which theoretically it “should” be), however, some companies label their products as “dairy-free” when really they are only lactose free, so always read the ingredients to be sure.
Also, a product can be casein-free but still contain lactose or even dairy fat. The challenge with casein-free foods is that there can be trace amounts, or there can be other components in the dairy that can cause problems, such as the milk sugar (lactose) or another protein. Many times people have a harder time processing the casein protein rather than the sugar or fat from dairy, but at least in the beginning, removing all components of dairy gives you a good look at whether there are reactions.
And in addition to the differences between the various components of milk itself, there are differences between different types of milk. A2 beta casein milk and camel milk, for example, but for the purpose of a dairy-free/casein-free diet (especially at the beginning) there is no animal milk of any kind included.
Autism and Diet
The signs of autism in children can be wide-ranging, such as avoiding eye contact, delayed language skills, sensitivity to sound, repetitive behaviors, and obsessive interests. Additionally, children with autism often have physical symptoms, such as gastrointestinal distress, diarrhea, constipation, sleep challenges, and rashes. And while these symptoms are not considered part of their autism diagnosis according to the DSM V, there is plenty of research showing that most children with autism struggle with these symptoms.
Following a therapeutic diet plan based on the unique needs of the child can reduce, or in some cases even alleviate, both autism symptoms and physical ones.
The body and brain are connected, so as you heal the body you improve health, learning, and behavior.
After we talk about the basics of what a gluten-free and dairy-free diet is, I’d like to share the science of WHY an autism diet like this works.
Tips to Consider…
While a gluten-free casein-free diet is not the only “autism diet” out there, it’s the best place to start for most kids. So for the purpose of this article I will call this diet the “autism diet.” But my overall nutrition philosophy and approach is about personalized nutrition (what I call BioIndividual Nutrition), because there is no one-size-fits-all diet. Instead, an optimal plan is tailored to the individual needs of each child.
Because there are so many negative reactions associated with gluten and dairy, and because people see such beneficial results (when they are omitted), it’s the first therapeutic diet I often suggest to people when getting started.
Here are some insights about implementing an autism diet plan:
Safe and Effective
Dietary intervention is something families can implement immediately. Parents are largely in control of what their child eats and can have a big influence on progress that can be made from a healthy gluten-free and dairy-free diet.
Improving your child’s food intake: Removing the harmful stuff and things devoid of nutrients and adding nourishing food over time… has no downside. Nutritional intervention is a safe and effective strategy.
In this VIDEO, Dr. James Adams, PhD explains nutritional intervention and our published study.
Review Your Child’s Diet for Gluten and Dairy Products
This approach omits all gluten and casein protein from your child’s diet…which isn’t an easy task. But with a little planning and follow through you can do it. Thoroughly reviewing your child’s diet is the first step in determining which foods to eliminate and which ones to leave alone.
However, gluten is also found in non-food products, such as Play-Doh, hygiene products, and it’s also in the adhesive on stickers and stamps. So be sure to think about the various ways your child may come in contact with products that may contain gluten.
Beginning a Gluten-Free and Dairy-Free Diet
There are generally two approaches for implementing a gluten-free and dairy-free diet. You can “dive in head first,” or you may prefer to follow a gluten-free diet first, then progress to dairy-free foods or vice versa. Either approach can work, as it’s up to you to determine the best option for your child and family.
I urge parents to be realistic in the time it will take to get familiar with all of the sources of gluten and/or dairy. Changing the way your child eats means changing the way you cook, so make sure you give yourself ample time to become familiar with all of those sneaky gluten or dairy ingredients.
In fact, in the GFCF diet implementation process I teach parents in my step-by-step nutrition program, the first half of the steps are things to help you get prepared before you even begin the diet.
While it may seem daunting at first, it gets easier over time, especially when you have the right support.
Soy-Free too!
Gluten and casein proteins are very inflammatory to the gut, they are two of the most common food allergies/intolerances, and they form opioid compounds when not fully digested.
Soy also has these problematic characteristics. So when implementing a gluten-free and casein-free diet, I almost always recommend removing soy as well. Technically speaking, the diet I recommend is a GFCFSF diet, However, because wheat and dairy are the main staples in the modern western diet and because it’s pretty easy to avoid soy, for simplicity I tend to refer to it as a GFCF Diet – though it’s really GFCFSF – gluten-free, casein-free, and soy-free.
What CAN Your Child Eat?
Following a gluten-free and dairy-free diet gives your child the flexibility to choose from various foods, like chicken, red meat, fruits, vegetables, eggs, nuts/seeds, beans, rice, potatoes, and anything that doesn’t contain casein or gluten. As you begin, you’ll start to notice there are many naturally gluten-free and dairy-free foods already in you or your child’s diet.
Reading food labels carefully is vital to avoid accidentally giving your child foods with gluten or casein proteins, as these ingredients are sometimes “hidden” in packaged products.

Benefits of a Gluten-Free and Dairy-Free Diet
Implementing an autism diet can offer immense benefits to your child. As noted earlier, improvements can be varied and include receptive and expressive language, enhanced cognition, better sleep cycles, less hyperactivity, improvements in constipation, and a decrease in disruptive behaviors.
The Science Behind a Gluten-Free and Dairy-Free Diet
Understanding the science behind an autism diet plan is important.
Many well-meaning friends, family members, therapists, and even health practitioners, may try to steer you away from this approach. Most often it’s from lack of knowledge, so the more knowledge you have the more you can advocate for your child and stay motivated in the face of any negativity. It will also help you speak more knowledgeable with your healthcare professional so you can know when they have an important medical point or when they are being dismissive because of their own lack of scientific understanding.
As we discuss the science behind gluten and dairy, in addition to the multitude of effects gluten and casein can have on the brain directly, also pay particular attention to inflammation–both in the gut and brain. Inflammation is at the root of most diseases and disorders. Inflammation of the brain is found in autism, as well as other neurological conditions such as ADHD, anxiety, depression, and more. It can cause many of the symptoms of autism. Additionally in the gut, inflammation affects our ability to digest our food properly and prevents us from absorbing the nutrients we need for our brain to function.
7 Science-Based Reasons Gluten and Casein Negatively Affect Autism (and the Research Behind It)
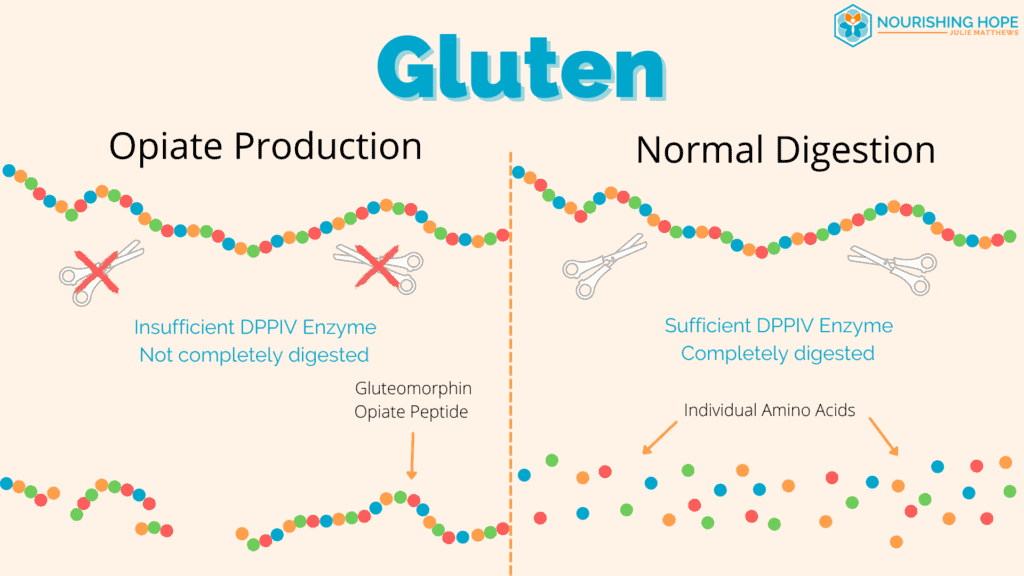
1. Opiates from Gluten and Casein in Autism
Did you know that certain long-chain peptides are very similar in structure to natural opioid-binding peptides? Gluten and casein are two such proteins. In fact, gluteomorphin, also known as gliadorphin, is the name of the opiate peptide formed during the (partial) digestion of gluten and casomorphin is the opiate peptide of dairy.
These peptides can enter the bloodstream for a few reasons. One of the first reasons is that the body needs adequate enzymes to break down these proteins and specifically an enzyme called DPP-IV. Children with autism have been shown to have lower DPP-IV activity. [1]
Another way these peptides can get into the bloodstream has to do with something that is called “leaky gut.” Leaky gut is a condition where the intestines become permeable, allowing things from the gut into the bloodstream, and leaky gut is common in autism. [2] When that happens, these peptides can bind to opiate receptors in the brain and create a whole range of issues such as high pain tolerance and even feeling foggy or disconnected. It can also create addictive-like behaviors to foods with these compounds. Many parents report that their child prefers to eat mainly foods with gluten, or dairy, or both. And this is also why when removing these from the diet, there can be symptoms like withdrawal. And some families report that their child’s restrictive eating improves once the gluten and dairy are out of their child’s system!
Here is more research on the opioids in foods and how they affect autism symptoms:
- Gluten and casein cause opioids excreted in urine, which affect behavior in autism. This study states, “A gut-to-brain axis is both possible and probable” [3]
- Epidemiological studies have linked the consumption of A1 beta-casein with neurological disorders, such as autism and schizophrenia [4]
- Exorphins (gluten-morphins and casomorphins) are found in the urine of people with autism [5]
- Gliadorphins and casomorphins can affect the neurotransmitter system in the central nervous system (CNS) and result in the social impairment seen in autism [6]
Opioids cause inflammation in the gut and brain. They also affect the brain directly, causing many symptoms including pain, irritability, anxiety, foggy thinking, and other symptoms common in autism, as well as addiction to gluten and dairy foods.
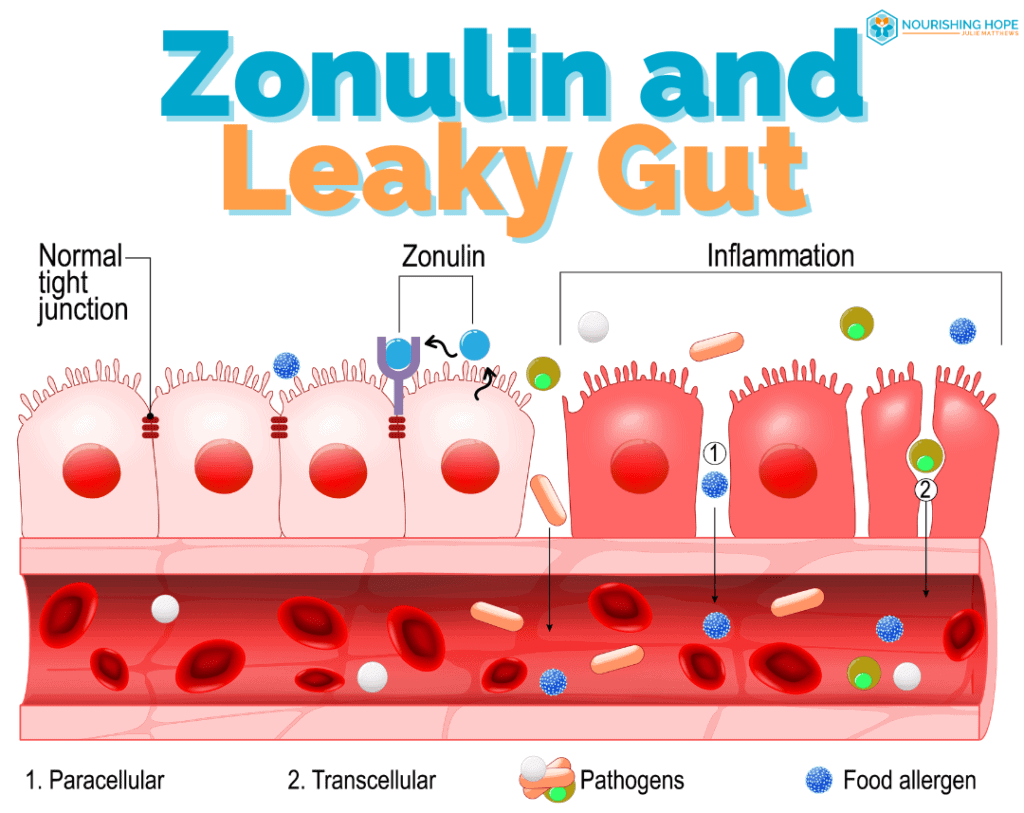
2. Zonulin and Its Role in Leaky Gut in Autism
Another advantage of implementing this diet is that gluten is known to trigger zonulin. Zonulin is a protein that modulates the permeability of the GI tract, and causes it to “unzip” or open, also known as,”leaky gut.” Studies show zonulin has been linked to gut permeability in autism, [7, 8] as well as many chronic inflammatory disorders (including autoimmune, metabolic, digestive, cancer, and neuroinflammatory). [9]
An increase in gut permeability can cause heightened reactions to other food components in the intestinal tract for children with autism. This can result in constipation, diarrhea, inflammation, food allergies/intolerances, or trouble concentrating. Since the gut and brain are connected, when the gut is unhealthy, the brain can’t function optimally.
We know individuals with autism have a higher prevalence of gastrointestinal (GI) issues. In fact, here is a blog I wrote about this almost a decade ago. And in a study by Dr. James Adams, the severity of gastrointestinal symptoms has been linked to the severity of autism symptoms. [10]
The above study on zonulin from 2021 [8] showed that serum zonulin was significantly higher in children with severe autism than controls. This suggests the missing link from Dr. Adams on the correlation between GI severity and autism severity may possibly be related to increased intestinal permeability.
Kids following a gluten-free diet have a much lower intestinal permeability than those who consume gluten.
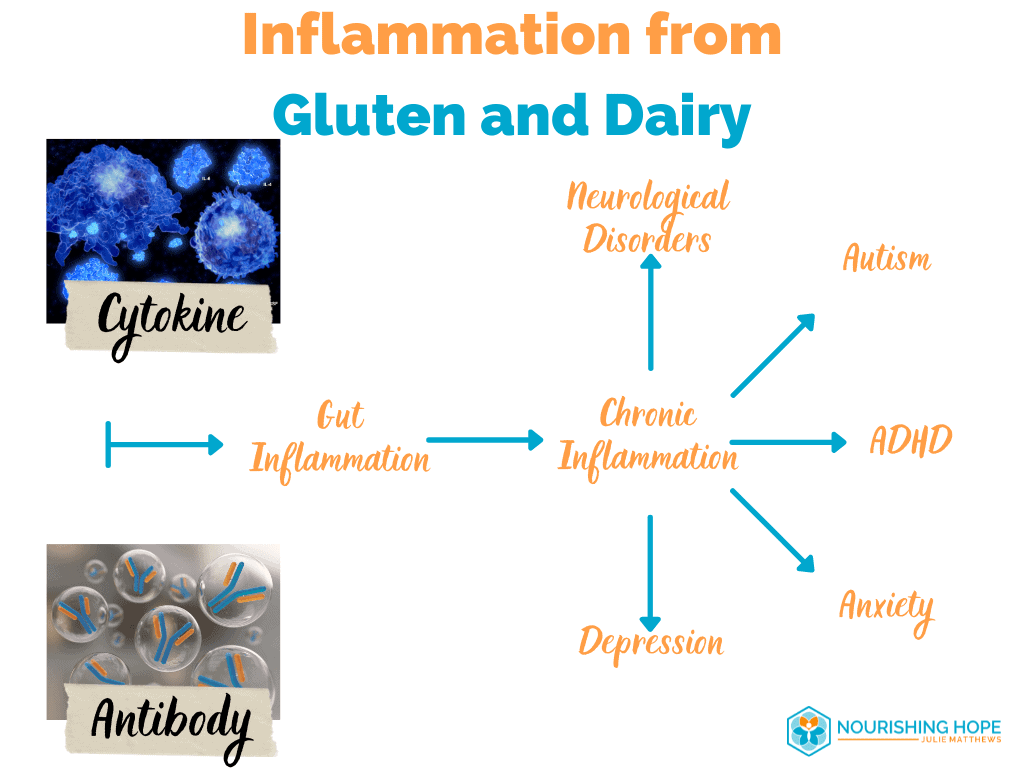
3. Inflammation to Gluten and Dairy in Autism
IgG antibodies to foods create inflammation in the body and in the gastrointestinal tract. In autism, researchers found high titer IgG antibodies to gliadin (gluten) in 87% of individuals with autism (as well as 86% of of those with schizophrenia) and high IgG antibodies to casein in 90% of people with autism (and 93% of schizophrenic patients). [11]
In another study, elevated inflammatory markers (cytokines) to gluten were found in people with ASD (Autism Spectrum Disorder) who had GI symptoms. [12]
Inflammation as a result of gluten and dairy can create issues in the gut and gastrointestinal symptoms such as diarrhea, constipation, gas, and pain. And in turn, this can cause systemic inflammation that affects the brain, as well as the negative effects caused by not breaking down our nutrients properly to get the nutrition our brain and body need.
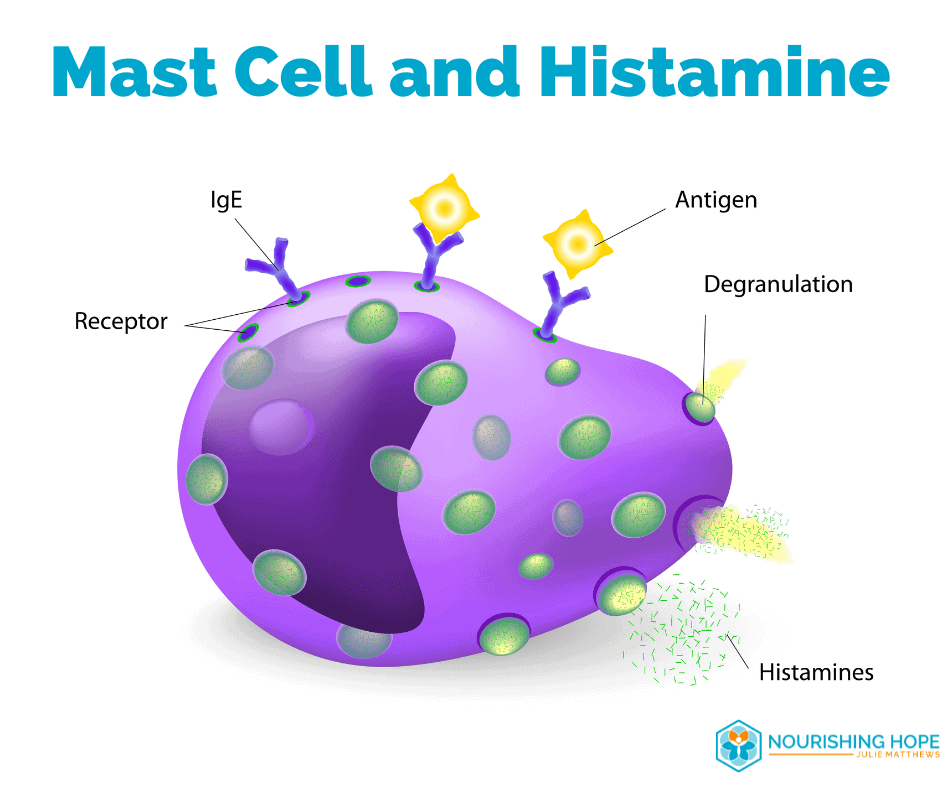
4. Mast Cell Activation in Autism
Mast cell activation and high histamine levels are common in autism, and research suggests this activation leads to inflammation in the brain (and locally in the gut) and is a possible cause in the development of autism. [13]
Food allergies, as well as gluten and casein intolerance [14], can cause histamine release. High histamine in turn can contribute to gastrointestinal disorders [15] and high acid levels in the stomach and GERD. And conversely histamine can increase food allergies.
Gastrointestinal disorders and high histamine in autism lead to increased symptoms and severity of ASD.
5. Increased risk of Celiac in ASD
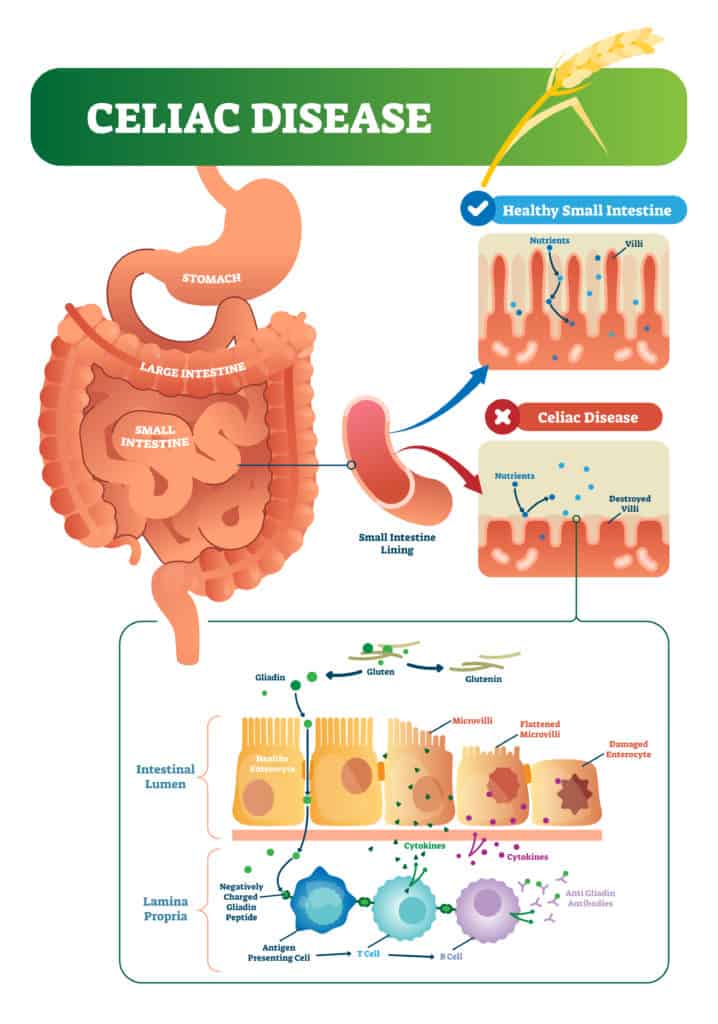
Celiac disease is an autoimmune reaction to gluten, where the body attacks the lining of the digestive system, causing severe digestive symptoms, as well as additional health conditions. While much of what we see in autism is non-celiac gluten intolerance, there is also an increased risk of celiac disease in autism.
Research shows that people with ASD are more likely to carry the HLA gene with the HLA-DRB1 *11-DQB1*07 structure, which increases the risks of celiac disease. [16]
6. Gluten, Casein, and the Glutamate Connection
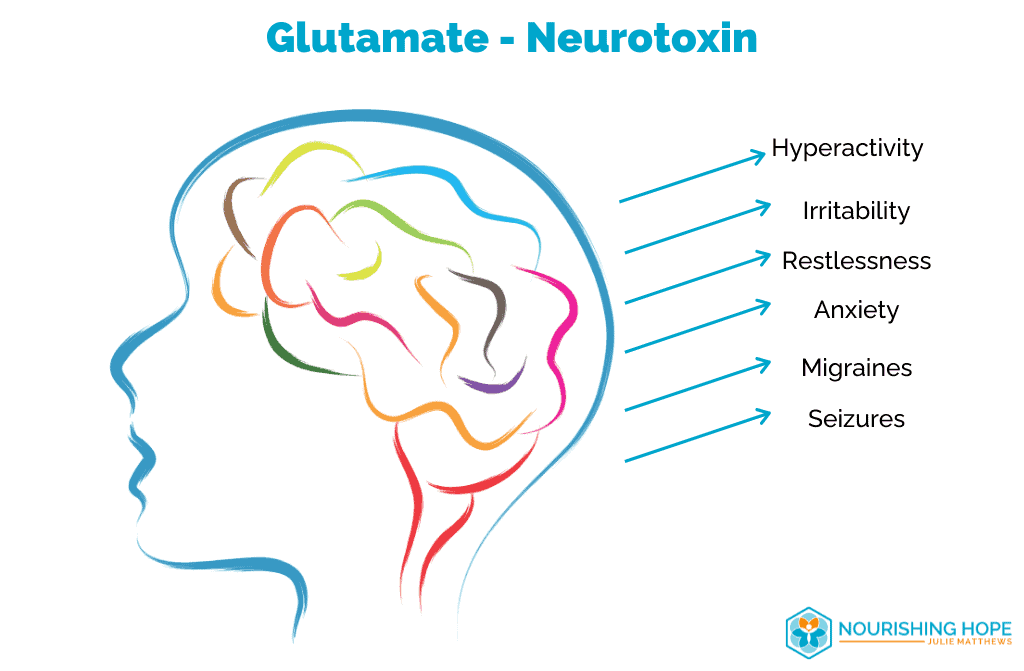
Glutamate is an excitatory neurotransmitter and some children (and adults) with autism are more sensitive, and their brains are more responsive to the effects of glutamate. That can result in more hyperactivity, irritability, restlessness, anxiety, migraines, seizures, and many more symptoms. Recent studies also show that elevated glutamate is often found in people with autism. [17]
Gluten is 25% glutamate by weight, and casein is 20%. Hence, gluten and casein in a diet can increase glutamate levels. And in sensitive people or those with high levels of glutamate such as those with autism, these foods can exacerbate neurological symptoms, including irritability, stress, anxiety, and hyperactivity. Glutamate can also cause inflammation in the brain and gastrointestinal system. [18]
Limiting the intake of gluten and casein in a diet can help reduce symptoms related to autism.
7. Dairy and Cerebral Folate Deficiency
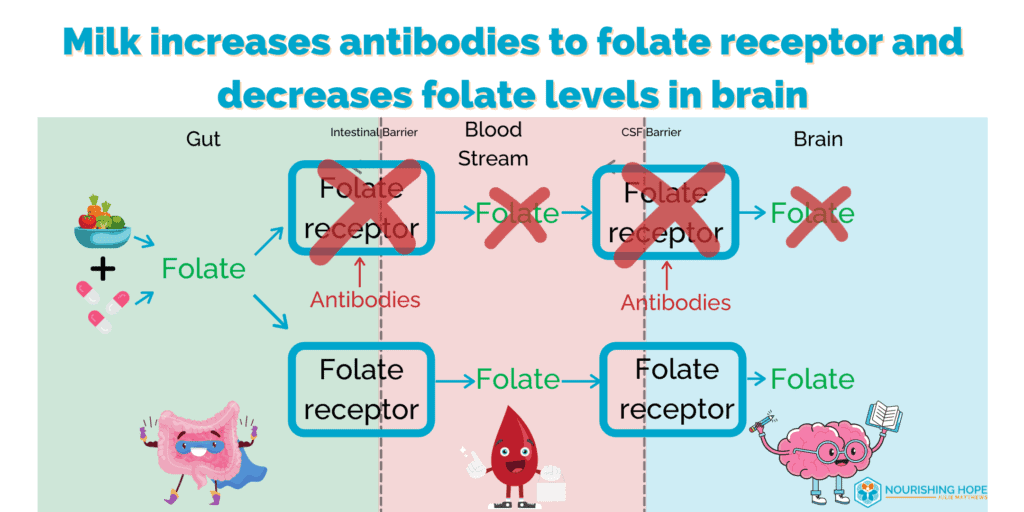
Some children with autism have a condition known as Cerebral Folate Deficiency. In this condition, folate is not able to be transported properly into the brain because of autoantibodies to the folate receptor, and there are not adequate levels of folate in the brain. This can lead to irritability and sleep problems, low muscle tone, slow head growth, loss of bodily movement, speech complications, and seizures.
One study showed that 75.3% of children with autism had folate receptor autoantibodies. [19]
Studies show that soluble folate-binding proteins in milk can cross react with folate receptors, increasing autoantibodies to folate receptors making this problem even worse for kids with autism by further decreasing folate to the brain. Conversely, studies show a dairy-free diet can reduce folate receptor autoimmunity in cerebral folate deficiency syndrome. [20]
A milk-free diet decreases folate receptor antibodies and autoimmunity.
Scientific Studies Showing Improved Symptoms and Positive Results from Gluten-Free Casein-Free (GFCF) Diet
Above I’ve shared the underlying factors that cause gluten and dairy to be a problem for people with autism. Below I share the growing scientific literature on the efficacy and benefits of a gluten-free and dairy-free diet.
91% of Children with Autism Improved Behavior, Speech, and/or GI on GFCFSF
 Research suggests that ASD may be accompanied by inflammatory immune responses, and that this may predispose people with autism to be more sensitive to the protein in wheat, dairy, and soy. Sensitization to these dietary proteins then leads to inflammation of the digestive system and exacerbates negative behaviors.
Research suggests that ASD may be accompanied by inflammatory immune responses, and that this may predispose people with autism to be more sensitive to the protein in wheat, dairy, and soy. Sensitization to these dietary proteins then leads to inflammation of the digestive system and exacerbates negative behaviors.
This exciting study resulted in 91% of the children showing clinical improvement that was observed by therapists/teachers/parents following implementation of a casein-free, gluten-free, and/or soy-free (cf/gf/sf) diet. Improvements were seen in GI symptoms, speech, autistic behavior, less hyperactivity, better focusing, and improved night time sleep. [21]
4.5x Developmental Age and 6.7 pts IQ from Diet and Nutrition Intervention in Autism
 This is a study I am particularly proud of because I was a part of it! Our study showed a 4.5x increase in developmental age as well as a 6.7 pts increase in non-verbal IQ. The study involved individuals aged 3-58 years old implementing a dietary intervention of a healthy gluten-free, casein-free, and soy-free diet; along with a multivitamin/mineral formula, essential fatty acid supplement, digestive enzymes, and a couple of additional nutritional interventions studied over one year. You can see my full write up on the study here.
This is a study I am particularly proud of because I was a part of it! Our study showed a 4.5x increase in developmental age as well as a 6.7 pts increase in non-verbal IQ. The study involved individuals aged 3-58 years old implementing a dietary intervention of a healthy gluten-free, casein-free, and soy-free diet; along with a multivitamin/mineral formula, essential fatty acid supplement, digestive enzymes, and a couple of additional nutritional interventions studied over one year. You can see my full write up on the study here.
In addition to improvements in development and IQ, major areas of improvement where seen across the board in included a reduction in autism symptoms and GI symptoms, improvement in language, focus, anxiety, and more. [22]
Reduced Autism Behaviors, Increased Social and Communication Skills with GFCF Diet
 This report reviewed existing scientific literature and found consistently positive results with a GFCF diet for autism. The literature included papers where groups of children were studied, as well as individual case studies.
This report reviewed existing scientific literature and found consistently positive results with a GFCF diet for autism. The literature included papers where groups of children were studied, as well as individual case studies.
Researchers found there was an overall reduction of autism behaviors, increased social skills, and communicative skills.
They also noted that autism traits reappeared after the diet had been broken. [23]
Development Was Significantly Better For the ASD Group On a GFCF Diet
 The aim of this study was to evaluate the effect of a gluten and casein-free diet for children with autism and on urinary opioid peptides associated with gluten, gliadin, and casein. The study found that the children who were on a gluten-free and dairy-free diet had better development than the controls. [24]
The aim of this study was to evaluate the effect of a gluten and casein-free diet for children with autism and on urinary opioid peptides associated with gluten, gliadin, and casein. The study found that the children who were on a gluten-free and dairy-free diet had better development than the controls. [24]
Given the prevalence of impaired social interaction, communication, and imaginative skills in autism, this study shows how powerful dietary changes can be!
Significant Improvement in Autism and ADHD Symptoms in Children with ASD on the GFCF Diet
 This study was a two-stage, 24-month, randomised, controlled trial with 72 Danish children (aged 4 years to 10 years 11 months) assigned to diet (A) or non-diet (B) groups. Autism Diagnostic Observation Schedule (ADOS) and the Gilliam Autism Rating Scale (GARS) were used to assess core autism behaviours, Vineland Adaptive Behaviour Scales (VABS) to ascertain developmental level, and Attention-Deficit Hyperactivity Disorder – IV scale (ADHD-IV) to determine inattention and hyperactivity. At 12 months, there was a significant improvement to the diet group scores on all autism, behavior, and ADHD scales measured. Because of the improvement in group A, group B was also assigned to the diet midway through the trial! The results suggest that dietary intervention may positively affect developmental outcomes for children diagnosed with ASD. [25]
This study was a two-stage, 24-month, randomised, controlled trial with 72 Danish children (aged 4 years to 10 years 11 months) assigned to diet (A) or non-diet (B) groups. Autism Diagnostic Observation Schedule (ADOS) and the Gilliam Autism Rating Scale (GARS) were used to assess core autism behaviours, Vineland Adaptive Behaviour Scales (VABS) to ascertain developmental level, and Attention-Deficit Hyperactivity Disorder – IV scale (ADHD-IV) to determine inattention and hyperactivity. At 12 months, there was a significant improvement to the diet group scores on all autism, behavior, and ADHD scales measured. Because of the improvement in group A, group B was also assigned to the diet midway through the trial! The results suggest that dietary intervention may positively affect developmental outcomes for children diagnosed with ASD. [25]
GFCF and Keto Diets Improve Autism Symptoms
 One study compared the GFCF diet to the Ketogenic diet for autism. Both diet groups had significant improvement in autism symptoms. There were some differences–one diet showed better results in behavior, while the other diet group had better scores for cognitive awareness and sociability. If you want to see more on this study, you can check out my GFCF vs. Keto write up. In summary, the results of this study showed that they are both good diets to improve symptoms of autism, depending on the individual needs of the person. And this study highlights another example of how the GFCF diet can benefit individuals with autism. [26]
One study compared the GFCF diet to the Ketogenic diet for autism. Both diet groups had significant improvement in autism symptoms. There were some differences–one diet showed better results in behavior, while the other diet group had better scores for cognitive awareness and sociability. If you want to see more on this study, you can check out my GFCF vs. Keto write up. In summary, the results of this study showed that they are both good diets to improve symptoms of autism, depending on the individual needs of the person. And this study highlights another example of how the GFCF diet can benefit individuals with autism. [26]
Closing Thoughts
Following a gluten-free and casein-free diet can help alleviate autism symptoms.
Creating an autism diet plan in advance can help you implement a GFCF diet smoothly and successfully.
Making these adjustments to your child’s diet can improve their symptoms of autism while also offering additional health benefits.
In fact, parents in my Nourishing Hope for Healing Kids program complete surveys at the end of the program. In the families that participated, 88% had improvement in their autism symptoms. Additionally, a majority had improvements in picky eating, cognition, play skills, expressive language, comprehension, attention/focus, aggression, GI symptoms, sociability, and more. This step-by-step program helps families implement a healthy GFCFSF diet along with additional personalized dietary strategies and nutritional supplementation
The encouraging news is that dietary intervention for autism can be an effective way to make dramatic improvements in your child’s health, learning, and behavior! The GFCF diet is a great intervention on your road to nourishing hope.
Download my GFCF Guide to learn more on implementing a gluten free and dairy free diet, or join us and other families just like you in our step-by-step nutrition program for parents and individuals.





Hello Julie,
How long this diet should be tried to evaluate changes?
Thank you!
Hi Emily, Typically a few months is a good timeframe to assess GFCF diets.
After reading your book we implemented a gfdf diet in 2018, however we have only now realised that an error made by our local health store (that we failed to spot) has meant we were using a bath soap that contain hydrolized milk protein as a final ingredient.
Do you normally recommend your clients to cease transdermal contact as well?
Thank you
Hi Julie, for people resistant to trying the gfcfsf, is it helpful to run the zonulin or urinary morphin testing? We’re high values on these tests tied to the improvement?
Great Article!
This is a great question, Julie! Studies show zonulin can be high in autism and urinary exorphins are high. There have been studies on gluten and casein opioids in autism and then the use of the GFCF diet, and results showed improvement. I don’t believe there has been a study yet looking at a GFCF diet in autism when zonulin is high. But that’s a great marker for a future study!
Thank you for such a well written explanation! It certainly helps to know with certainty that the effort it takes to implement a gfcfsf diet is truly worth it.
Not only that but so filled with HOPE!!!
Thank you for sharing your knowledge this article will definitely help me speak more convincingly. I am grateful.
Betsy, I’m so happy about that. At Nourishing Hope I certainly strive to nourish hope. I’m glad this article did so, and was helpful as well. All the best to you!
Hi Julie, thank you for a thorough report on this. How about raw milk or raw kefir. I put my son on a GFCf diet but each time I take out kefir I see he goes backwards so I put it back in and we have more sleep. Whats the take on raw milk? And why do some people see results on this?
Thank you for the GF Diet for Children.
Question – Any recommendation for adults with in the early stage of Dementia, cognitive memory decline?
Thank you for your response.