Nutritional and dietary intervention is effective at improving non-verbal IQ, autism symptoms, developmental age in children and adults with ASD.

I’m very excited to share the results of a new scientific study on autism: this is my first published paper!
You read that right! I am one of the co-authors of this study, which was led by James Adams, PhD, entitled “Comprehensive Nutritional and Dietary Intervention for Autism Spectrum Disorder—A Randomized, Controlled 12-Month Trial.”[1]
Dr. Adams is the director of the Autism/Asperger’s Research Program at Arizona State University, where he has been studying this condition for the past 15 years. He’s also the father of a daughter with autism.
Five years ago, Dr. Adams approached me and my colleague Dana Laake to help with a study on autism; specifically researching how nutrition and diet can improve the symptoms of autism. He asked that we contribute to the research by educating and guiding participants how to implement a healthy GFCF diet, which was a core intervention of the study.
The Highlights
As a nutritionist specializing in Autism Spectrum Disorder, I’ve been investigating the unique physiology, etiologies, and “bioindividual” biochemistry in people with ASD since 2002; specifically, how food and nutrition choices affect the body and behavior (symptoms) in autism, and how to devise individualized therapeutic diet strategies that help alleviate these symptoms. I’ve witnessed significant improvements in the health and happiness of children with ASD using special diets and nutritional supplementation; from modest digestive improvement to complete recovery. Regardless of the degree to which the person with autism recovers, we see improvement, across the board, with a healthy, gluten free, casein free, soy free diet.
This study supports what many practitioners and parents have been seeing in practice all along. Finally, we have conclusive evidence that nutritional and dietary intervention is effective at improving non-verbal IQ, autism symptoms, and developmental age in children and adults with ASD! There were improvements in anxiety, mood, aggression, hyperactivity, focus, and more!
Thus, I’m thrilled to share the results of this 1-year comprehensive study with all of you. The outcomes were life changing for many of the children that participated, and their families and communities, too.
And there were some stunning recoveries. One study participant recovered so quickly through treatment that she no longer has to use her wheelchair! Simply from dietary and nutritional approaches, another boy no longer has to be catheterized! Other stunning results from this study include: eliminating pica (eating non-food items which can be life threatening) in two children, improving symptoms of autism, helping them connect more with loved ones, and having a better quality of life… all of which were found from this research.
Furthermore, the hope that it brings to the rest of us: that this simplifed approach is safe, accessible. and doable for any autism family!
This study should greatly influence the medical and educational community regarding treating those with autism: for awareness and progress is so necessary, as most doctors are poorly informed. Even the Academy of Nutrition and Dietetics (formally the ADA) erroneously indicates that there “not enough science to support dietary intervention for autism.”
In this article, I’ll discuss the details in this recently published study, and clarify how we used specific supplements with an allergen-free diet, to address the most common etiologies and co-morbidities within the ASD subpopulation.
Who was included in the research?
A total of 117 individuals, aged 3 to 58, enrolled in the study. None of them had taken nutritional supplements (vitamins, minerals, essential fatty acids, carnitine) or consumed “special” diets in the previous two months.
67 of the participants had been previously diagnosed with ASD (autism, Pervasive Developmental Disorder-Not Otherwise Specified (PDD-NOS), or Asperger’s). Arizona State University staff verified the participant’s ASD diagnosis using the Autism Diagnostic Observation Schedule (ADOS) and/or the 2nd edition of the Childhood Autism Rating Scale (CARS-2).
The remaining 50 participants were neurotypical, meaning that none of them had been diagnosed with a mental disorder including ASD, ADHD, depression, or anxiety. Moreover, none of these participants had a first-degree relative with ASD.
How was the study conducted?
The study was designed as follows:
Assessment of ASD symptoms
After enrollment, autism severity and overall functioning level were assessed among participants with ASD. ADOS, CARS-2, Reynolds Intellectual Assessment Scales (RIAS), or Severity of Autism Scale (SAS-Pro) were utilized during the evaluation.
Moreover, parents or high-functioning adult participants filled in a medical history form at the beginning of the study. They also completed various questionnaires at the beginning and end of the intervention to assess autism and related symptoms.
Random Assignment
The participants with ASD were then randomly assigned to either the ASD treatment group or to the ASD Non-treatment group as outlined below:
- The treatment group consisted of 37 participants (30 males and 7 females). This group was composed of 28 children (ages 3 to 12), 6 teenagers (ages 13 to 20), and 6 adults (over 20 years old).
- The non-treatment group included 30 participants (25 males and 5 females). This group consisted of 20 children, 7 adolescents, and 3 adults.
The neurotypical group consisted of 41 males and 9 females (34 children, 11 teenagers, and 5 adults).
Health and Biomarker Assessments
The study physician physically examined all the participants to ensure that they were sufficiently healthy to participate in the research.
First-morning urine and blood samples were collected once at the start of the study in the neurotypical group and at the beginning and end of the study in the treatment and non-treatment groups and.
These samples were sent for analysis to commercial laboratories approved by the Clinical Laboratory Improvement Amendments (CLIA) program.
The blood biomarkers measured included:
- Ammonia
- Lactic acid
- Creatine Kinase
- C-Reactive protein
- Thyroid panel (TSH, T3, T4)
- Complete Blood Count (CBC)
- Red blood cells (RBC) minerals and fatty acids
- Homocysteine-related metabolites (homocysteine, cysteine, methionine)
Treatment protocol
Only participants in the ASD treatment group received the combined treatment protocol.
Participants in the non-treatment group were promised that they would obtain all the supplements and diet advice once the study was completed. The only condition was that they made no significant change to their nutritional therapy, medical treatment, or education treatment for 12 months. This step helped reduce drop-outs.
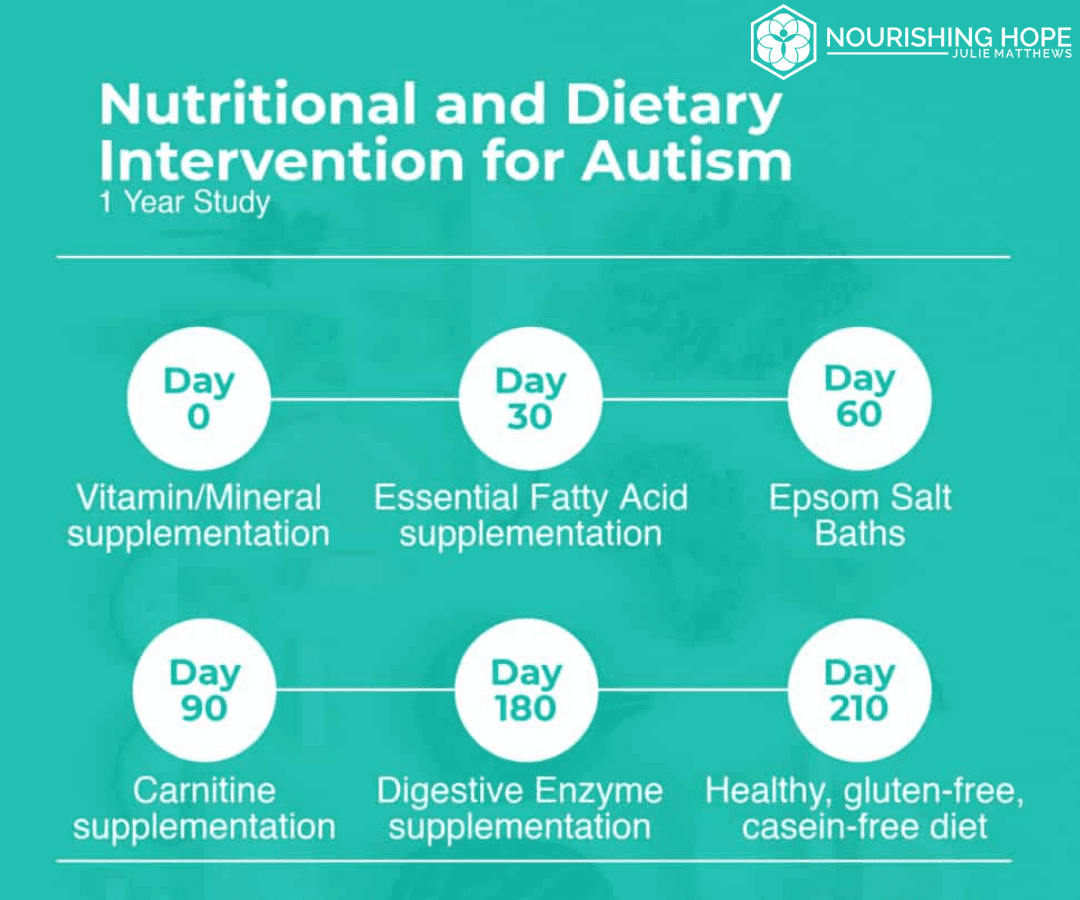
The treatment group started treatment with a multivitamin/mineral supplementation. The dose was adjusted based on the child’s weight and split into 3 doses (breakfast, lunch, and dinner).
On day 30 of the study, the participants received an essential fatty acid supplement containing 609mg omega-3’s (425mg EPA, 110mg DHA, 74mg other omega 3’s), 198mg omega-6 (including 128mg GLA), and 15mg omega-9. The participants started with 1 capsule daily and then increased to a maximum of 4 capsules daily depending on their weight.
On day 60, participants were asked to take one warm Epsom salt bath for 20 minutes, twice a week. Two cups of Epsom salts and half a cup of baking soda were added to the bath.
On day 90, participants started taking 50mg of acetyl-L-carnitine/kg bodyweight-day. This dosage was gradually increased to a maximum of 2 grams/day over 4 weeks and split into two doses (breakfast and dinner).
On day 180, the participants were advised to take a plant-based digestive enzyme supplement. The dose was as follows:
- 1 capsule for a snack or small adult meal
- 2 capsules for a typical adult meal
- 3 capsules for a large adult meal
On day 210, the participants started a healthy, gluten-free, casein-free, soy-free (HGCSF) diet outlined below.
All the supplements and dietary changes were continued until the end of the study.

Why this protocol?
- Vitamins/minerals: As mentioned earlier, individuals with ASD have profound nutritional deficiencies which can have deleterious effects on overall health and ASD symptoms. Supplementation can help increase several biomarkers and vitamin status.
- Essential fatty acids (EFAs): These fatty acids help maintain cell membrane health. It is, therefore, no surprise that an EFA deficiency could adversely affect brain health and lead to depression and psychological disorders.But did you know that our intestines need EFAs to function correctly? In fact, an EFA deficiency could explain why supplementation can help improve GI symptoms that are common in ASD.
- Epsom salt baths: Epsom salts are magnesium sulfate salts and have been found to be highly effective in increasing plasma sulfate levels. Healthy sulfate levels are required for optimal detoxification, synthesis of healthy brain tissue, intestinal and brain barrier function, neurotransmitter and gastrointestinal functions.
- Acetyl-L-carnitine: Carnitine is involved in energy metabolism and mitochondrial protection. This compound helps remove potentially harmful substances from the mitochondria and cell so that they can be excreted from the body. In previous research, Dr. Adams found that individuals with ASD who supplemented with carnitine scored better on scales that assessed severity of autism symptoms and global functioning [4].
- Digestive enzymes: Gastrointestinal symptoms can predict autism severity. Digestive enzymes enhance digestive function and alleviate gastric upset, thus relieving pain and associated autistic behaviors, as well as improving nutrient absorption and nutrition levels.
- HGCSF diet: If not properly digested, gluten, casein, and soy can favor the production of opiates, which can fit opiate receptors in the brain. This can cause brain fog, trouble concentrating, constipation, and inflammation. Moreover, gluten, casein, and soy can increase intestinal permeability – this can severely affect the gut-brain axis.
Besides removing potential food triggers, the HGCSF diet also aims to heal cells throughout the body (including the gut) by reducing inflammatory proteins, support detoxification pathways, and strengthen the immune system.
My role in this study
Dana Laake and I were the two nutritionists on the team of 15 other medical professionals and academic researchers. I really enjoyed working with Dana – she’s very collaborative, passionate and knowledgeable. I’ve known this lovely person for years, and I’m very impressed with her super smart nutrition brain. Dana is also the author of two successful books.
So, for this study, Dana and I designed a 1-hour power point presentation with audio for the families of the participants in the treatment group. The presentation aimed to help these families better grasp:
- What the HGCSF diet is all about
- The science, or what we called the [numerous] “whys” behind the diet
- How to implement the HGCSF diet easily
- How to assess the effectiveness of this diet
Dietary changes recommended in this study
In a nutshell, the intervention group was advised to:
- Consume a nutrient dense diet with adequate organic produce, quality protein, and sufficient calories from healthy fats like coconut oil, olive oil, ghee (certified casein-free if no dairy IgE allergy), and grass-fed tallow.
- Remove food toxins that place extra burden on detoxification pathways (like MSG, artificial flavors, colors, and preservatives) by avoiding processed foods.
- Remove foods that promote gut inflammation (such as gluten, casein, soy, sugar, and industrial seed oils).
Now, that you know everything there is to know about this study, let’s discuss the study’s findings.
Findings of this study
Improvements in cognitive, GI function, and medical biomarkers
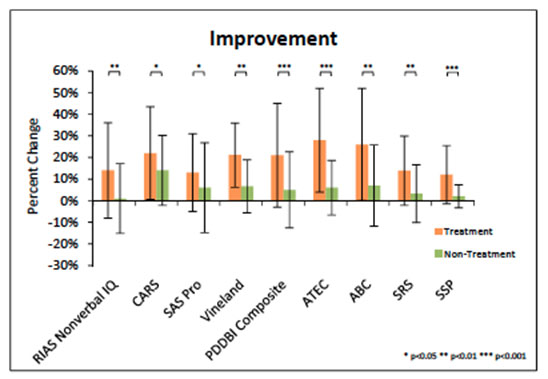
Compared to the control group, the treatment group experienced significant changes in:
- Cognitive function as indicated by considerable improvements in non-verbal IQ tests with gains of 6.7 IQ points.
- The treatment group ‘gained an average of 18 months of development’ with substantial progress in communication, social, and daily living skills. This was 5 times the development over the control group. They also performed significantly better on all of the ASD/behavioral assessments.
- Gastrointestinal symptoms: Constipation and diarrhea improved as well as stool smell.
- Carnitine levels increased in the treatment group.
- Fatty acids levels: DHA and EPA levels increased in the treatment group. Levels of arachidonic acid decreased and could result in a reduced production of pro-inflammatory molecules.
- Red blood cell minerals: Selenium and chromium levels increased in the treatment group.
- Homocysteine pathway: The combined treatment helped reduce homocysteine levels to normal.
- Vitamins: Levels of vitamin B2, B5, folic acid, CoQ10H2, one vitamin B6 biomarker, and cyanocobalamin (a form of vitamin B12) improved in the treatment group
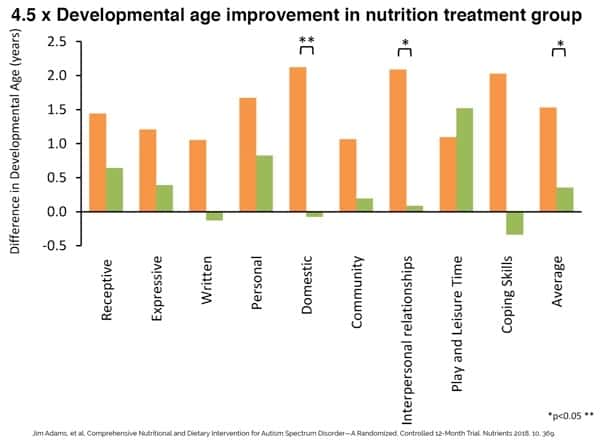
Improvements in mood, behavior, and focus
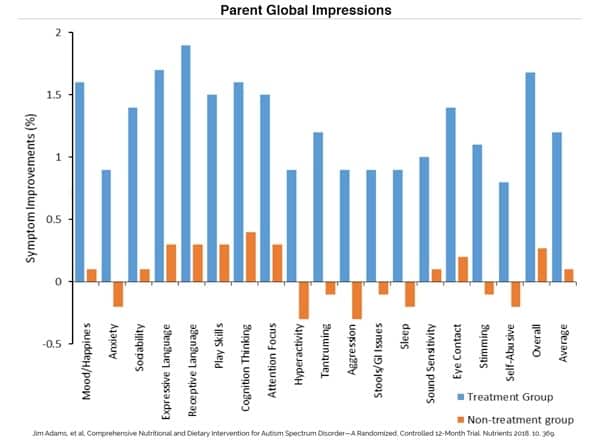
There were significant improvements in the diet and nutrition treatment group based on Parent Global Impressions. These included statistically significant improvement in:
- Mood/happiness
- Anxiety
- Sociability
- Attention focus
- Hyperactivity
- Tantrums
- Aggression
There were three exceptional cases
hree participants in the treatment group also showed remarkable improvements:
- A 7-year-old boy with pica was healed entirely within one week of starting the HGCSF diet. Pica is the eating of non-food items like rocks, twigs, or batteries, and it can be very dangerous.
- A 27-year-old male with severe ASD and a history of severe urinary retention requiring daily catheterization was able to urinate on his own after only 4 days eliminating dairy products. By the end of the study, the young man no longer needed catheterization and had zero episodes of kidney stones, urinary tract or bladder infections.
- One 9-year-old girl with severe ASD had poor strength, endurance, and energy levels at the beginning of the study. Four months after the treatment, she no longer needed her wheelchair. We found out that her pre-treatment diet was deficient in carnitine due to total avoidance of beef and pork products, so supplementation showed to be critical for her strength and stamina.
Some adverse effects were observed
The following treatments caused a few reactions:
- Vitamins/Minerals: Two brothers experienced a moderate worsening of behavior and stopped all supplements after 4 months. They did, however, benefit from the HGCSF diet which cured severe pica for one child.
- Carnitine: This supplement made one child “feel sick” and was discontinued by the parent.
- Digestive enzymes: The enzymes caused intestinal symptoms in one child who discontinued use after one month. Extended use of this supplement triggered facial rash in another participant who eventually decided to stop taking it despite noticing improvements in behavior and constipation.
- HGCSF diet: Removing one child’s favorite foods led to frustration and caused behavioral problems as well as an inability to solve problems.
There is No Magic Window
Some people believe in a “window” for treatment, that the older an individual gets the less likely treatment will help. This study proves that wrong! And thank goodness!
It’s always bothered me that people would think that, because I have found it not to be true – and that people of all ages can improve. After all, our message behind “Nourishing Hope” doesn’t exclude anyone, no matter their age or diagnosis. I certainly believe no one should dash the hope of older children and adults unnecessarily and erroneously.
The study found under Age Effects, “An evaluation of changes on all the outcome measures suggests that there was no significant correlation of benefits with age, so children and adults of all ages are likely to benefit from this combination treatment.”
Implementing nutritional and dietary intervention at any age is worthwhile. It’s never too late to be nourishing hope.
Additional insights
- L-carnitine may be better absorbed than acetyl-l-carnitine.
- Some vitamins that did not increase significantly during the study, such as vitamin D, may be needed in larger doses and/or more bioavailable forms to have a therapeutic value.
What does this research confirm
1. Autism is a whole-body disorder and the brain is downstream
Autism has long been considered as a cluster of psychiatric/psychological behaviors caused by defective genes that induced structural changes in the brain before birth. However, current research clearly shows that autistic individuals have suboptimal biochemical pathways that affect neurological function.
For example, a majority of children with autism have issues with:
- Methylation which is responsible for controlling DNA synthesis, building neurotransmitters (brain chemicals), and enzyme production. This pathway also ensures that neurons fire in sync. It also helps the body create ATP (or cellular energy).
- Transsulfuration, which is the primary part of the body’s innate detoxification system, depends on a healthy methylation pathway.
- Sulfation which helps the body eliminate toxins by binding them to sulfates. This renders the toxins more water-soluble and, hence, safer to excrete. Sulfation relies on methylation and transsulfuration.
So, as you can imagine, if any of these pathways are ‘broken,’ a cascade of symptoms will occur. For example, individuals with autism often suffer from:
- Digestive issues
- An inflamed gut
- Decreased detoxification
- Increased intestinal permeability
- An imbalanced gut flora (with too many pathogens and few beneficial bacteria)
All of these symptoms can significantly impact the brain since they impair nutrient absorption, cause oxidative stress, and increase inflammation. The good news is that various studies show that supporting these pathways can considerably improve ASD symptoms.
2. Individuals with ASD are severely deficient in various nutrients
As I have mentioned in a previous article, multiple studies indicate that child
ren with ASD often have deficiencies in:
- Vitamins

- Essential fatty acids
- Sulfate
- Digestive enzymes
- Antioxidants like glutathione
These studies also indicate that supplements can correct these deficiencies and alleviate ASD symptoms.
3. Food sensitivities are common in autism
Studies have shown that children with ASD often have abnormal immune responses to:

- Gluten (in wheat, rye, oats, barley)
- Casein (from dairy products)
- Soy (not always)
In one study, 81% of children who eliminated gluten and casein for 1 year improved considerably [2]. These improvements continued over the next 12 months!
What kind of study was this?
This research used a single-blinded approach where the clinical evaluators, but not the participants, were blinded. What this means is that only the participants knew whether they were receiving the combined intervention or no treatment at all.
Since clinical evaluators are blinded, this approach eliminates the possibility of bias or manipulation of results during assessments and laboratory measurements. A single-blind study is also more realistic and practical and better mimics real-world implementation. It also reduces the possibility that participants will drop out of the study.
I proudly assert that this study followed the strictest scientific rigor for research of its kind, and that it’s findings are credible. Some diet naysayers may dismiss the current study, arguing that it’s not the “gold standard” of a randomized, double blind, placebo controlled study, or that it studies too many variable at once.
Firstly, when dealing with whole foods, it is very difficult, or nearly impossible, to conduct a double-blind study (one in which both the evaluators and the participants are blinded). The participants are eating real food and need to know what they are eating; anybody would agree, it’s hard to get around that. Secondly, with multiple interventions being used, it more closely depicts how most families conduct a dietary intervention and nutrition program. Families are not going to try one intervention, wait a year and then try the second, and the third, etc. And there is synergy among diet and nutrient treatments: vitamins and minerals are co-factors for each other enhancing their individual effects, and diet and nutrients also have improved results when used together.
What sets this study apart?
Why did we conduct this study when previous studies already indicate that dietary changes and specific nutritional supplements can improve ASD symptoms?
Well, these earlier studies looked at either the effects of diet or nutrition therapy individually and over a short period of time. None of them investigated whether combining these two treatments over the long-term could be more efficient.
So what sets this study apart?
Comprehensive approach
Since autism is a whole-body disorder, combining a comprehensive nutritional intervention with specific dietary modifications could be more effective in improving many ASD symptoms.
Duration of the study
Individuals with ASD often use supplements over an extended period. And the effects of nutritional interventions are often slower than those of pharmaceutical interventions.
Therefore, we conducted this research over 12 months to assess the long-term effects of this combined approach on ASD symptoms among adults and children. The long duration of the study also allowed for a more extensive evaluation of possible adverse effects.
Quality of supplements used
Dr. Adams has improved the vitamin/mineral supplements used in this study based on findings from his previous research [3]. The new and improved version of the supplement contains:
- A higher dose of vitamin D, niacin, pantothenic acid, biotin, selenium, mixed tocopherols.
- Added vitamin K, potassium, carnitine, vanadium, and boron.
- A lower dose of manganese, molybdenum, lithium.
Note: Dr. Adams makes no money from the sale of the supplements used in the study.
Quality of study design
This study utilized a very robust study design, as described below, to ensure that the findings are reliable and not due to chance or bias.
Takeaway Message and Conclusion
- Combining nutritional supplements and dietary changes is safe and efficient at improving ASD symptoms.
- Even adults with autism can improve with nutritional and dietary intervention.
In my opinion, future studies may yield ever greater results with a more refined bioindividual approach. For example, certain approaches like carnitine did not offer noticeable improvements for a majority of the participants, but for those that it did, like the girl in the wheelchair, it was life changing. While this study wasn’t looking at this specifically, customizing a nutritional approach to the biochemical and individual needs of the person, can likely yield even more beneficial results.
The study’s conclusion says it all, “The positive results of this study suggest that a comprehensive nutritional and dietary intervention is effective at improving non-verbal IQ, autism symptoms, developmental age, and other symptoms in most individuals with ASD, with the vitamin/mineral supplement, essential fatty acids, and healthy HGCSF diet reported by parents to be the most beneficial.”
It was an honor to be part of this study. The finding supports the clinical results I have been seeing in my clinical nutrition practice for the past 16 years. And this study helps support clinicians and parents all over the world that want to use a diet and nutrition approach to help children and adults with ASD
Now, I’d love to hear from you: have you tried any of the supplements or dietary changes described in this study? If so, it would be wonderful if you could share your experience in the comment section below. I’m sure your feedback could help others take the lead.
By Julie Matthews
References
1. Adams, J.B.; Audhya, T.; Geis, E.; Gehn, E.; Fimbres, V.; Pollard, E.L.; Mitchell, J.; Ingram, J.; Hellmers, R.; Laake, D.; Matthews, J.S.; Li, K.; Naviaux, J.C.; Naviaux, R.K.; Adams, R.L.; Coleman, D.M.; Quig, D.W. Comprehensive Nutritional and Dietary Intervention for Autism Spectrum Disorder—A Randomized, Controlled 12-Month Trial. Nutrients 2018, 10, 369.
2. Cade R, Privette M et al. “Autism and Schizophrenia: Intestinal Disorders” Neurosci 3 (2000) 57-72. Published by Overseas Publishers Association, (OPA) N.V.
3. Adams JB, Audhya T, Mcdonough-Means S, Rubin RA, Quig D, Geis E, Gehn E, Loresto M, Mitchell J, Atwood S, Barnhouse S, Lee W Effect of a Vitamin/Mineral Supplement on Children with Autism, BMC Pediatrics 2011, 11:111
4. Geier DA, Kern JK, Davis G, King PG, Adams JB, Young JL, Geier MR. A prospective double-blind, randomized clinical trial of levocarnitine to treat autism spectrum disorders. Med Sci Monit 2011 Jun;17(6):PI15-23.





Would this supplement be beneficial for a child who has been diagnosed with ADHD?
I can’t say whether something would be right for an individual. But generally speaking a high quality multivitamin/mineral formula can be helpful for most people. And my experience shows that there are some similarities on nutrients that are beneficial between autism and ADHD.
I put my daughter on the GFCFSF diet in Julie’s Nourishing Hope Diet when she was non-verbal and 4 years old. I had noticed that my daughter gravitated to macaroni and cheese, dairy, chicken McNuggets, etc and when she ate these foods she seemed like she was on a high from drugs and her behavior became terrible. Julie’s book explains why they crave certain foods and why there is an opiate affect on their brains. I learned how to make healthy foods for her body and brain from Julie’s Cooking to Heal cookbook. Her books changed the trajectory of my daughter’s life. I am happy to report Katie is very verbal and appears neuro-typical to most, but is on ASD spectrum. She is doing well in school and therapies. I can’t thank you enough for your education and books. I am an advocate and nurse for children with special needs, with specialty in ASD. I tell parents about these books and have seen the testaments to these diets in many children. Thank you Julie!!
Christy, thank you for sharing this wonderful story of your daughter! <3 I'm so glad she is doing well. Thank you for the feedback on how my work has helped you all. It's so touching. You have made my day. All the best to you and your daughter.
How wonderful to see such dramatic and positive results from a diet modification. What a breath of fresh air to see a health problem considering our bodies’ ability to heal themselves given a chance. Hopefully, your study triggers more research to follow. I feel it is the tip of the iceberg and you are touching on this when you mention bio individuality. One cannot help but think that diving deeper into the micro biome is only logical especially considering the widely known impact of the gut on brain functionality not to mention the gene expression from our micro biome outnumbering our own 1:100 (check my numbers, I could be wrong). It has also been found that people with autism have a very poor microbiome which explains the gut issues and the different reactions to supplementation which, again, highlights that bio individuality factor to your study. Maybe stool testing should be added to your protocol.
Just a thought, I’m sure you get a lot of those. Thank you for all you do. You are bring hope to so many people. Sincerely,
Marielle, Thank you for the thoughtful response and your ideas. These are great facts and points. I do plan to do more research, so I’ll consider all this as I continue my research journey.
It is wonderful that you were able to do such of great study, and that you were able to obtained the majority of results you were expecting. I am glad you were able to probed that good healthy diet interventions and supplementation could change the daily path of kids ASD and other. Congratulations
Hi,
My 3 year old ASD son is already on a multivitamin and fish oil plus takes Epsom salts baths. I really want to follow your protocol so should I stop the fish oil and baths and reintroduce them on the stipulated days?
Many thanks.
Thank you so very much Julie for everything you’ve generously presented here!
It appears that your study has made a unique and vital contribution to the field of nutrition therapy.
Would it be reasonable to summarize your food recommendations as: a “Nourishing Traditions” diet minus the casein and gluten? ……… If so have you presented this to the Weston A. Price Foundation? ……… There are thousands of members who could appreciate this as well!