 It has long been known by parents (and many health professionals), that children with autism have higher prevalence of gastrointestinal (GI) issues. Ask any parent of a child with autism, and they will likely tell you that their child has gastrointestinal symptoms: diarrhea, constipation, gas/bloating, or pain.
It has long been known by parents (and many health professionals), that children with autism have higher prevalence of gastrointestinal (GI) issues. Ask any parent of a child with autism, and they will likely tell you that their child has gastrointestinal symptoms: diarrhea, constipation, gas/bloating, or pain. Regrettably, digestive symptoms like diarrhea, constipation, and bloating are often ignored or considered an aspect of a child’s “autism.” This suggests that somehow diarrhea and other potty accidents are a “behavior,” and result of autism. This is preposterous.
After years of study, research is confirming that GI problems are higher in children with autism (see chart below).
 A research study in the journal BMC Gastroenterology, explored not only “if” children with autism are different, but “how.”
In this study, “Gastrointestinal flora and gastrointestinal status in children with autism–comparisons to typical children and correlation with autism severity,” Dr. Jim Adams, found differences between the children with autism and controls, and also found that GI distress appears to play a role in autism symptoms.[1]
The study concluded, “The strong correlation of gastrointestinal symptoms with autism severity indicates that children with more severe autism are likely to have more severe gastrointestinal symptoms and vice versa.”
Before we go into more about what the research found, I have put the summary of studies Adams, et al. outlines in the “Background” section into a chart to layout the research that identifies an increase of GI problems in children with autism.
Children with Autism Have Increased Rates of GI Distress
A research study in the journal BMC Gastroenterology, explored not only “if” children with autism are different, but “how.”
In this study, “Gastrointestinal flora and gastrointestinal status in children with autism–comparisons to typical children and correlation with autism severity,” Dr. Jim Adams, found differences between the children with autism and controls, and also found that GI distress appears to play a role in autism symptoms.[1]
The study concluded, “The strong correlation of gastrointestinal symptoms with autism severity indicates that children with more severe autism are likely to have more severe gastrointestinal symptoms and vice versa.”
Before we go into more about what the research found, I have put the summary of studies Adams, et al. outlines in the “Background” section into a chart to layout the research that identifies an increase of GI problems in children with autism.
Children with Autism Have Increased Rates of GI Distress
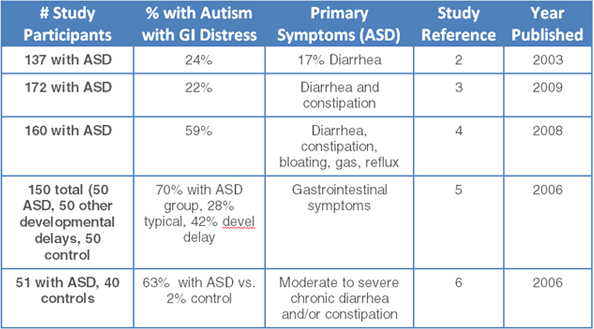 Adams, et al. in BMC Gastroenterology
You can see that there are many studies showing an increase in digestive disturbances with children with autism. Back to the study itself and the findings. Children with autism had:
Adams, et al. in BMC Gastroenterology
You can see that there are many studies showing an increase in digestive disturbances with children with autism. Back to the study itself and the findings. Children with autism had:
- Beneficial Bacteria: The children with ASD had much lower levels of bifidobacterium and much higher levels of lactobacillus.
- Inflammation: The only marker that showed a significant difference was lower level of lysozyme in the autism group. “A marker consistent with bacterial, viral, allergenic, and autoimmune caused bowel inflammation.” The researchers suggest “possibly associated with probiotic use.”
- Short Chain Fatty Acids: There was a significantly lower amount of SCFA as a total, as well as lower levels of acetate, proprionate, and valerate in the group with autism. It was suggested to be due in part by probiotic use (as the children with autism taking probiotics had the greatest lowest SCFA values), as well as lower intake of fiber, and other reasons.
- Adams, J. B., Johansen, L. J., Powell, L. D., Quig, D., & Rubin, R. A. (2011). Gastrointestinal flora and gastrointestinal status in children with autism–comparisons to typical children and correlation with autism severity. BMC gastroenterology, 11(1), 22.
- Molloy CA, Manning-Courtney P: Prevalence of chronic gastrointestinal symptoms in children with autism and autistic spectrum disorders. Autism 2003, 7(2):165-171.
- Nikolov Roumen N, Bearss Karen E, Jelle Lettinga, Craig Erickson, Maria Rodowski, Aman Michael G, McCracken James T, McDougle Christopher J, Elaine Tierney, Benedetto Vitiello, Eugene LArnold, Bhavik Shah, Posey David J, Louise Ritz, Lawrence Scahill: Gastrointestinal Symptoms in a Sample of Children with Pervasive Developmental Disorders. J Autism Dev Disord 2009, 39:405-413.
- Xue Ming, Michael Brimacombe, Janti Chaaban, Barbie Zimmerman-Bier, Wagner George C: Autism Spectrum Disorders: Concurrent Clinical Disorders. J Child Neurol 2008, 23(1):6-13.
- Valicenti-McDermott M, McVicar K, Rapin I, Wershil BK, Cohen H, Shinnar S: Frequency of gastrointestinal symptoms in children with autistic spectrum disorders and association with family history of autoimmune disease. J Dev Behav Pediatr 2006, 27(2 Suppl):S128-36.
- Adams JB, Holloway CE, George F, Quig D: Analyses of Toxic Metals and Essential Minerals in the Hair of Arizona Children with Autism and their mothers. Biol Tr El Res 2006, 110:193-209.



If this was all that is causing it then there shouldn’t be any kids left with autism. The fact that some kids have a hard time eating in the first place is very alarming. I just think the truth is not being told, and we are being told more excuses. How can anyone keep looking at this, and not think something is terribly wrong considering how many kids keep being affected by autism is beyond me.
Dr Bradstreet has written about how probiotics “like” an aerobic environment, rather than an anaerobic environment, such as the small and large intestines. So, from what he has stated about probiotics, I am not surprised at the results about probiotic use.
Thank you for this article. There are certain GI MDs in my area that need to read it. My son was not offered an EGD by an MD at Children’s Memorial in Chicago b/c of his “autism” diagnosis. My son has severe oral aversions. Once I took him to Dr. Arthur Krigsman, my son finally had a full scope done of his GI tract, and we got some answers. (EE and Crohn’s like ileitis.)
I hope that many autism parents will bring this article to pediatric GI MDs who blame GI issues on behavioral components of autism. Our kids have physical problems in their GI tracts.
Correction: only the large intestine is an anaerobic environment.
“Regrettably, digestive symptoms like diarrhea, constipation, and bloating are often ignored or considered an aspect of a child’s “autism.” This suggests that somehow diarrhea and other potty accidents are a “behavior,” and result of autism. This is preposterous.”
Well, it’s preposterous with the assumptions you make. 🙂 I completely agree that diarrhea/constipation/potty accidents are not behavioural. But I disagree about it being a result of the autism. Autism is not a behavioural issue. It’s not psychological. Behaviours AND the potty problems are both the result of the autism, which is a neurological issue.
Hi Luna,
I agree. Originally, I had written something similar explaining that if you see “autism” as neurological – it is a result of autism. I decided to simplify it for the purposes of this article. Next time, I’ll explain that point as well. Thanks for the feedback.
If it’s neurological, then why did a neurologist not know a thing about my son’s aspergers? No clue how to diagnose it. I went to a children’s behavioral specialist to get his diagnosis. Shouldn’t a neurologist know about all branches of autism? Including aspergers?