
Insights into the influence of dietary changes on symptoms of autism are providing families with more hope than ever before.
Autism has long been considered a “mysterious” brain disorder that begins/ends in the brain, and that affects observable social behavior.
But autism is far more than a behavioral-only diagnosis; it is a whole-body disorder. Whether it’s the common inflammation, digestive problems, or sleep issues they experience, these physical symptoms of autism affect the overall health of autistic children.
I believe from my extensive research on developmental disorders that a targeted autism diet can improve children’s quality of life and may be simpler than you think to start.
Autism intervention requires more than what traditional therapies and medications offer or provide. Supplying the body what it needs to engage natural healing processes by avoiding problematic foods and adding healthy foods is crucial to the health of your child. In this article, I demystify an “autism diet,” explain why dietary intervention works, and how to start your child on this safe and natural approach..
Top 4 Areas to Address with Diet
Autism is a whole-body disorder. The foods and substances that are fed to children directly impact what happens in their brain… and can impact the symptoms of autism.
There are many body systems and biochemical processes that need to work properly for the body to be healthy and the brain to function well — they require nutrients, a normal inflammatory response, good cellular and metabolic function, proper digestion, and adequate detoxification.
Special diets can put the puzzle pieces together and give parents the information you need on your journey of nourishing hope. As I stated, diet can help a myriad of autism symptoms, and here are four top underlying factors that targeted diet plans can help.
1. Leaky Gut & Inflammation
This is one of the most widespread and common symptoms of autism that can be addressed with diet, and I write about tummy aches often.
Leaky gut and inflammation can be extremely painful for a child, even exacerbating behavioral problems as they will try anything to ease these painful issues in the digestive tract. Behavior, rashes, and language issues all improve with reduced inflammation and better gut health.
Leaky gut, or “intestinal permeability,” is a condition in which the layer of cells protecting the intestines are compromised and can leak waste or other particles into your bloodstream. This is harmful because only certain particles are meant to be absorbed from the intestine and sent into circulation.
To combat this issue of inflammation and leaky gut, I recommend you steer clear of sugar, refined oils, soy, corn, and eggs. Even more importantly, ditch the gluten and casein, proteins found in wheat derivatives and dairy products.
All of these foods, especially gluten and casein, feed into inflammation. Unfortunately, they are a major part of the Standard American Diet.
After you’ve knocked out what’s feeding the problem, add in some positive elements. Try fermented foods like sauerkraut, dairy-free yogurt, or kefir to increase your amounts of good bacteria.
Prebiotics like bananas, beans, garlic, and more will also increase the good bacteria already living in your gut. Finally, try out some anti-inflammatory food choices like turmeric, ginger, and fish oil to help heal the inflammation that’s gotten out of control.
2. Nutrient Deficiencies
Children with ASD frequently experience nutrient deficiencies. This can be due to a number of factors like picky eating, when asked to try new foods. The inflammation and leaky gut mentioned above can also make it difficult to properly absorb nutrients.
A well-nourished child is a healing child, and there are several things that can be done to support this process. First, increase the quality of food, increasing your child’s food intake of organic products and grass-fed meats. More vegetables are also vital for improving nutrient levels. If your child won’t try them, try pureeing or juicing to make things easier.
Finally, consider using supplements. Vitamins, minerals, and fatty or amino acids are all acceptable forms of nutrients. Working closely with a nutritionist or dietitian on an autism diet, as well as with your child’s doctor, can help to remedy your child’s individual nutritional deficiencies.
3. Imbalanced Microbiome
The microbiome is a term that refers to the balance of bacteria in your body, both beneficial and pathogenic. One of our main sources of good bacteria is in the food that we eat, and your child’s diet can directly determine the quality of the microbiome and digestive tract. Scientific studies show that our microbiome, via the gut-brain axis, affects more than our gut, from brain function to stress levels.
One specific microbial culprit is yeast, and antibiotic use aids its growth as good bacteria no longer exist to crowd it out.
A diet to balance the microbiome will first remove sugar. Not only does it contribute to inflammation, but also feeds yeast and other pathogens in the body — whether from a sweet treat or too much fruit.
Next, you may want to remove yeast itself from your diet, which is often found in bread, aged meats and cheeses, and grapes. The last compounds to avoid when balancing the microbiome are refined starches, such as breads and gluten-free grains.
Along with these eliminations, add in fermented and probiotic-rich foods, which help with microbiome rebalancing along with the inflammation mentioned above. My book, Cooking to Heal, details ways you can ferment at home.
ment at home.
4. Biochemical Imbalances
Children with autism often have biochemical imbalances that stem from both genes and nutrient deficiencies. Studies show that children with autism are low in glutathione. Glutathione a primary detoxifier and antioxidant.
Toxins deplete our glutathione stores. And when toxins cross into the brain, tantrums and hyperactive behaviors may increase. Both boosting glutathione levels through nutrients and reserving it by avoiding exposure to toxins can help. One step you can take is to avoid food additives, which are difficult to process and harmful to our health. Aluminum and plastic are also difficult to remove from the body, and can transmit toxins from cooking and storage containers to the food being cooked.
To reduce your child’s exposure to toxins, eat organic foods, and avoid pesticides, GMOs, and hormones. Grass-fed meats, organic produce, and pastured chickens are all safer, natural options.
Finally, help the liver, which plays a major role in detoxification, by eating foods high in A, C, E, and B vitamins. Foods high in sulfur, such as cauliflower, broccoli, and Brussels sprouts, also support liver function and can be useful. Broccoli and broccoli sprouts are high sulforaphane: a nutrient that increases glutathione levels in the body and has been shown to improve autism symptoms.
Glutathione first requires proper methylation:a set of biochemical pathways that are impaired in the bodies of children with ASD. Methylation has hundreds of important functions in the body, including: healthy gene expression, proper mitochondrial function (i.e. energy production), good mental health, and the avoidance of leaky gut and anxiety.
Supplementing with nutrients like B6, B12, folate, magnesium, and zinc can help with methylation. You can work with your pediatrician and nutritional team to determine exactly which supplements your child needs for proper methylation.
Generally speaking, a healthy diet rich in folate, B vitamins, magnesium, zinc, sulfur, and other nutrients will help support these important biochemical pathways.
Gut-Brain Connection
As you can see, the foods we eat affect the brain.
Poor quality food can lead to deficiencies such as vitamins, minerals and fatty acids that are needed for brain function. Without proper nutrients the body can’t perform many tasks, including thinking clearly and paying attention.
When digestion is not working well, we can’t absorb nutrients well.
Certain foods such as wheat and dairy can cause inflammation in the gastrointestinal tract. This can lead to systemic inflammation, that negatively affects brain function.
Additionally, gluten (a protein in wheat), and casein (a protein in dairy) when improperly digested can create opioid compounds. These compounds cross the blood-brain barrier and fit in the opiate receptor (like morphine) and can cause very severe symptoms: such as: irritability, difficulty with language, insensitivity to pain, and even food cravings for these problematic foods.
Healthy Gluten Free & Casein Free Diet (GFCF)
A healthy gluten-free diet and casein-free is a great introduction to a specialized autism diet.
Gluten and dairy can cause intestinal inflammation, leaky gut, poor digestion, and tummy aches. And a healthy GFCF diet can help improve digestion and digestive symptoms such as diarrhea, constipation, gas, and bloating. And as your child’s gut heals, they can absorb more nutrients and begin to thrive.
I encourage parents to eliminate harmful food allergies, and to incorporate better healthy alternatives as well. While a gluten and casein-free diet may sound daunting for the parent of a picky eater, I assure you after supporting thousands of families, that it’s possible and the benefits are tremendous.
Educating yourself thoroughly before you start the diet, and having a clear nutrition plan (like mine) are key to success here.

Foods to Avoid
In its most straightforward form, gluten can be found in grains like wheat, rye, spelt, kamut, barley, and oats (except certified gluten-free oats).
However, gluten can be sneakier than that — it commonly hides in seemingly innocent items like sauces, spice blends, and flavorings. Reading the label is key to avoiding gluten.
Casein is also found in more than just milk, ice cream, and yogurt; it’s commonly lurking in chocolate, whey protein, potato chips, and even dairy-free cheese. Again, reading the food label is the only way to be sure. And remember to avoid processed foods and food additives.
One important thing to note is that the Standard American Diet relies on dairy for calcium, so be sure to add calcium rich-foods and/or supplementation to avoid deficiency.
Healthy Foods
As you remove gluten and casein, consider adding in a few healing, healthy alternatives. Try making your own non-dairy yogurt with coconut or nut milks and adding in some fermented foods mentioned above like sauerkraut or kefir.
Homemade bone broth is a dish that’s simple to prepare and can aid both digestion and healing; adding in vegetables can increase the mineral content even more.
And add lots of vegetables to your child’s diet. The vitamins, minerals, and phytonutrients will help support their biochemistry and needed functions.
Grain-Free Diet
 A grain-free diet like the Specific Carbohydrate Diet, GAPS Diet (Gut and Psychology Syndrome Diet), or Paleo Diet is a more refined dietary step. It avoids not only gluten-grains, but all grains (and starches like potatoes too).
A grain-free diet like the Specific Carbohydrate Diet, GAPS Diet (Gut and Psychology Syndrome Diet), or Paleo Diet is a more refined dietary step. It avoids not only gluten-grains, but all grains (and starches like potatoes too).
This autism diet is appropriate in more severe cases of inflammation, with IBS, or with children who have low carbohydrate enzymes (which is common in autism).
Grains are difficult to digest and can be a source of severe inflammation for children with gastrointestinal problems and an imbalanced microbiome.
SCD/GAPS Diet
The Specific Carbohydrate Diet (SCD) and GAPS diet remove all starches (polysaccharides) and complex sugars (disaccharides), and only allow monosaccharide carbohydrates (single sugar molecules). The GAPS diet is a version of SCD, so the food lists are very similar. These foods are avoided as they can be hard to digest for some individuals and can contribute to dysbiosis (imbalanced microbes) and cause inflammation and digestive symptoms. They also negatively affect the brain through the gut-brain-microbiome connetion.You can learn more about how these diets works here.
In a scientific study I published with Dr. James Adams, we found the SCD Diet improved attention in 24% of individuals with ASD, as well as cognition in 22%, and anxiety and diarrhea in 19%, among many other symptom improvements including irritability and language.
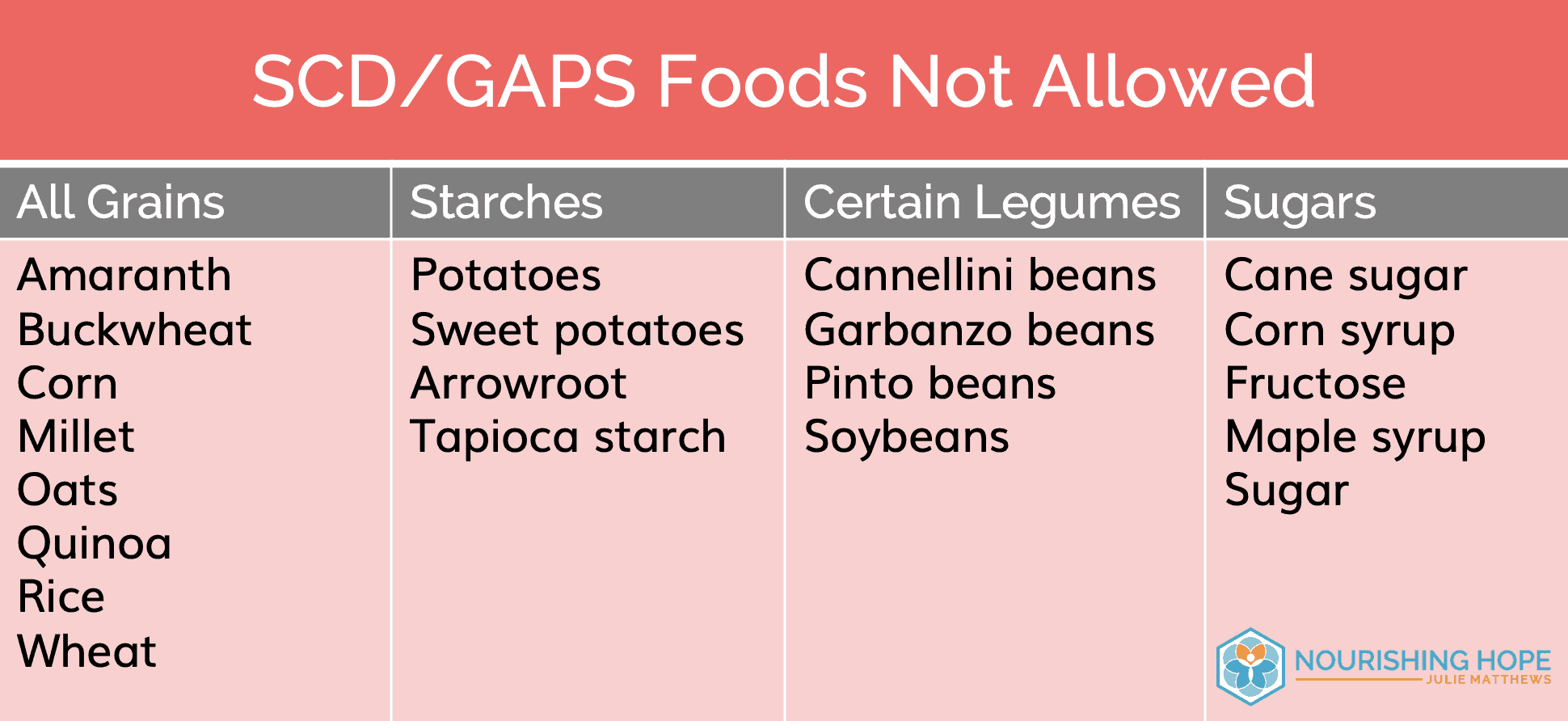
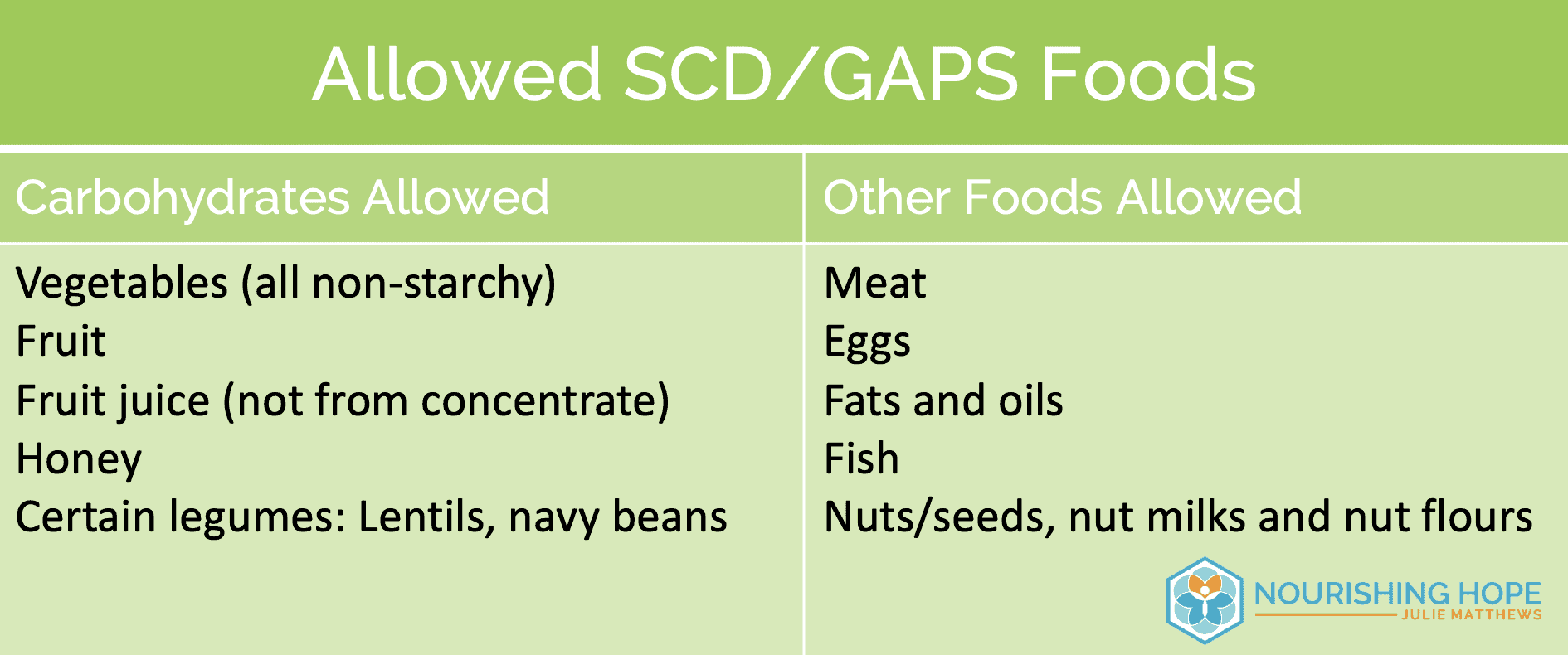
The SCD/GAPS diets are similar diets that limit carbohydrate intake to fruits and non-starchy vegetables, and a few legumes. The following is a list of foods allowed and not allowed on this diet.

Paleo Diet
The Paleo diet is another grain-free diet that can be helpful for individuals with autism.
This Paleo diet avoid:
- Grains
- Dairy
- Refined sugars
- Legumes
- Processed oils
It emphasizes meat, fish, vegetables, whole fruits, eggs, nuts, and seeds.
While a grain-free autism diet can be challenging to implement, it’s an excellent option when more significant dietary intervention is needed.
In Summary
- Parents are learning that an autism diet can be extremely beneficial in addressing ASD and its underlying conditions.
- An individualized autism diet can heal inflammation, rebalance the microbiome, and improve a variety of functions throughout the body.
- A GFCF diet avoids gluten and casein. This special diet, along with supplementation, is an excellent starting point for addressing autism spectrum disorder through diet.
- For more severe gastrointestinal situations, a grain-free diet can yield beneficial results.
- I have designed a helpful nutrition program designed to aid parents on their journey toward nourishing hope and healing their child through diet.
Sources
- Adams, J., Audhya, T., Geis, E., Gehn, E., Fimbres, V., Pollard, E., … & Matthews, J. (2018). Comprehensive nutritional and dietary intervention for autism spectrum disorder—A randomized, controlled 12-month trial. Nutrients, 10(3), 369. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5872787/
- Depino, A. M. (2013). Peripheral and central inflammation in autism spectrum disorders. Molecular and Cellular Neuroscience, 53, 69-76.
https://www.sciencedirect.com/science/article/abs/pii/S1044743112001856 - Chaidez, V., Hansen, R. L., & Hertz-Picciotto, I. (2014). Gastrointestinal problems in children with autism, developmental delays or typical development. Journal of autism and developmental disorders, 44(5), 1117-1127. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3981895/
- Devnani, P. A., & Hegde, A. U. (2015). Autism and sleep disorders. Journal of pediatric neurosciences, 10(4), 304. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4770638/
- Mu, Q., Kirby, J., Reilly, C. M., & Luo, X. M. (2017). Leaky gut as a danger signal for autoimmune diseases. Frontiers in immunology, 8, 598. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5440529/
- Iovene, M. R., Bombace, F., Maresca, R., Sapone, A., Iardino, P., Picardi, A., … & de Magistris, L. (2017). Intestinal dysbiosis and yeast isolation in stool of subjects with autism spectrum disorders. Mycopathologia, 182(3-4), 349-363. Abstract: https://www.ncbi.nlm.nih.gov/pubmed/27655151
- Adams, J. B., Audhya, T., McDonough-Means, S., Rubin, R. A., Quig, D., Geis, E., … & Barnhouse, S. (2011). Nutritional and metabolic status of children with autism vs. neurotypical children, and the association with autism severity. Nutrition & metabolism, 8(1), 34. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3135510/
- Matson, J. L., & Fodstad, J. C. (2009). The treatment of food selectivity and other feeding problems in children with autism spectrum disorders. Research in Autism Spectrum Disorders, 3(2), 455-461. Abstract: https://www.sciencedirect.com/science/article/pii/S1750946708001256
- Adams, J. B., Audhya, T., McDonough-Means, S., Rubin, R. A., Quig, D., Geis, E., … & Barnhouse, S. (2011). Effect of a vitamin/mineral supplement on children and adults with autism. BMC pediatrics, 11(1), 111. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3266205/
- Carabotti, M., Scirocco, A., Maselli, M. A., & Severi, C. (2015). The gut-brain axis: interactions between enteric microbiota, central and enteric nervous systems. Annals of gastroenterology: quarterly publication of the Hellenic Society of Gastroenterology, 28(2), 203. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4367209/
- James, S. J., Cutler, P., Melnyk, S., Jernigan, S., Janak, L., Gaylor, D. W., & Neubrander, J. A. (2004). Metabolic biomarkers of increased oxidative stress and impaired methylation capacity in children with autism. The American journal of clinical nutrition, 80(6), 1611-1617.
https://www.ncbi.nlm.nih.gov/pubmed/15585776 - Blaylock, R. L. (2009). A possible central mechanism in autism spectrum disorders, part 3: the role of excitotoxin food additives and the synergistic effects of other environmental toxins. Alternative Therapies in Health & Medicine, 15(2). Abstract: https://www.ncbi.nlm.nih.gov/pubmed/19284184
- Nieves, R., & Jackson, R. T. (2004). Specific carbohydrate diet in treatment of inflammatory bowel disease. Tennessee medicine: journal of the Tennessee Medical Association, 97(9), 407-407. Full text:
- https://jandonline.org/article/S2212-2672(15)00504-3/fulltextWilliams, B. L., Hornig, M., Buie, T., Bauman, M. L., Paik, M. C., Wick, I., … & Lipkin, W. I. (2011). Impaired carbohydrate digestion and transport and mucosal dysbiosis in the intestines of children with autism and gastrointestinal disturbances. PloS one, 6(9), e24585. Full text: https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0024585




0 Comments